More than half of GP practices believe the quality of care they deliver is deteriorating because of rising workload according to a new British Medical Association survey of almost 2,900 GP practices in England. The survey was answered by just over a third of GP practices in England, and asked about their current workload.
Key findings:
- Over half of GP Practices in England (55%) reported that the quality of service in their practice had deteriorated in the past twelve months.
- Just 2% of practices said their workload was low or generally manageable.
- More than half (55%) said their workload was unmanageable a lot of the time while just over one in ten (13%) said it was unmanageable all of the time
- Nine of ten practices (92%) aid that there had been a rise in demand for appointments in the past twelve months.
- The West Midlands had the highest level of unmanageable workload with sixteen percent of GP practices recording this level, while the South of England reported the biggest deterioration in patient care with two thirds of practices (66%) saying it had declined.
The BMA has produced a heatmap of Parliamentary constituencies showing the worst affected areas and will be 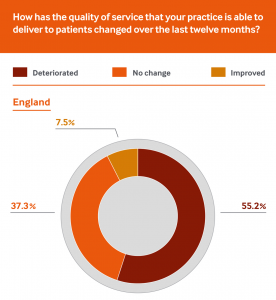 launching a new initiative for GP practices called an “Urgent Prescription for General Practice”.
launching a new initiative for GP practices called an “Urgent Prescription for General Practice”.
This will include sending every GP practice in England a package of support materials, including guidance on how to manage workload safely.
Dr Beth McCarron, BMA GP Executive team member said:
“These figures clearly show that general practice is in a state of emergency with the majority of GP practices across England registering a deterioration in the quality of care being delivered to patients.
“This is clearly the result of rising workload, including increasing patient demand for appointments which is placing unsustainable pressure on GP services that have been starved of resources and staff. There were more than 600 trainee GP positions left unfilled in 2015 at a time when a third of the workforce are considering retirement in the next five years. This comes at a time when GP practices are seeing 150,00 more patients each day than in 2010, but have seen no extra resources to maintain effective, safe care to the public. With an ageing population, this pressure is only likely to increase in the years to come.
“Politicians have to realise that general practice is currently running on empty. GPs desperately want to provide the best possible service for patients: this is why GPs became doctors. But we have to be given the tools and support to provide patients with the service they deserve. The government has to realise that we cannot go on with a crisis situation where sliding quality of care becomes an accepted part of general practice.”


